Key Takeaways
- Post-treatment aftercare directly affects healing speed, pigment stability, and surface texture after acne scar resurfacing.
- Sun exposure control is non-negotiable and influences pigmentation outcomes after laser procedures.
- Skincare product selection during recovery can either protect the treated skin barrier or trigger secondary irritation and complications.
- Activity restrictions and hygiene practices influence infection risk and scar remodelling following in-clinic procedures.
- Follow-up schedules at laser clinics in Singapore determine whether early complications are corrected or allowed to worsen.
Introduction
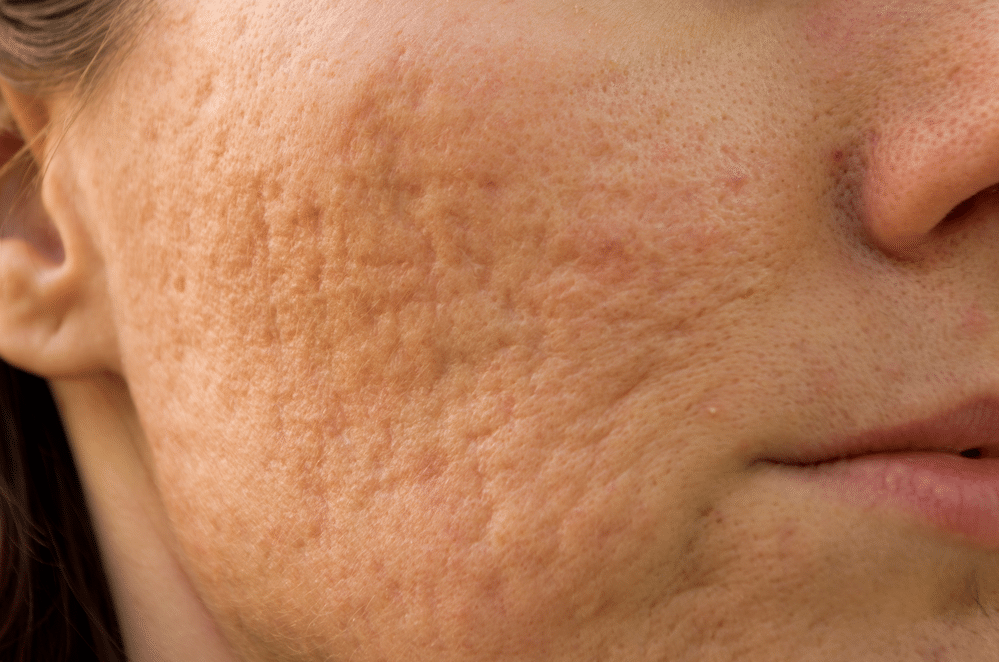
Acne scar resurfacing relies on controlled injury to the skin to stimulate remodelling and collagen repair. The clinical outcome does not depend on in-clinic energy settings alone. What happens after treatment determines how well the skin recovers, whether pigmentation changes stabilise, and whether secondary scarring or prolonged inflammation occurs. Laser clinics in Singapore routinely advise structured aftercare protocols because post-procedure behaviour directly affects treatment safety and results. Patients who do not follow aftercare instructions often experience delayed healing, uneven texture, persistent redness, or post-inflammatory hyperpigmentation, particularly in humid climates and high UV exposure environments.
1. Sun Avoidance and UV Protection Protocols
Sun exposure is a primary driver of post-inflammatory hyperpigmentation following acne scar resurfacing, especially in patients with medium to darker skin tones. Treated skin is photosensitive during the initial recovery phase, and unprotected UV exposure increases melanocyte activity while the epidermal barrier is compromised. Laser clinics commonly advise strict sun avoidance during the first two weeks, followed by ongoing broad-spectrum sunscreen use even when visible redness subsides. Patients who resume outdoor exposure too early often develop uneven pigmentation patches that require corrective sessions or pigment-targeted treatments later. Physical barriers such as wide-brim hats and avoidance of peak UV hours reduce cumulative risk, while inconsistent sunscreen application allows low-grade UV damage that may not be immediately visible but affects long-term resurfacing outcomes.
2. Product Selection and Skin Barrier Management
Post-procedure skin requires low-irritation support to maintain barrier integrity during epidermal recovery. Using active ingredients such as retinoids, exfoliating acids, scrubs, or fragranced products during the healing phase increases transepidermal water loss and prolongs inflammation. Acne scar resurfacing creates microthermal zones that depend on controlled re-epithelialisation, and improper product use disrupts this process. Laser clinics typically advise a simplified regimen of gentle cleansers, barrier-repair moisturisers, and medically appropriate occlusives where indicated. Patients who reintroduce acne treatments prematurely often experience delayed healing, surface roughness, and increased sensitivity that interferes with treatment sequencing. Barrier compromise also increases susceptibility to secondary infections, particularly in humid environments where sweat and occlusion are difficult to avoid.
3. Hygiene, Activity Restrictions, and Environmental Exposure
Post-treatment skin is vulnerable to microbial contamination and mechanical disruption. Touching treated areas, engaging in contact sports, using shared gym equipment, or exposing skin to pools and saunas introduces contamination risks that can trigger folliculitis, secondary acne flares, or superficial infections. Acne scar resurfacing outcomes are affected when inflammatory lesions develop during healing, as inflammation interferes with collagen remodelling and may produce new textural irregularities. Laser clinics often recommend avoiding intense physical activity, steam rooms, and swimming during early recovery to reduce moisture exposure and friction. Patients who resume these activities early report higher rates of prolonged redness and patchy healing, particularly when sweat accumulates on healing skin and disrupts epidermal closure.
4. Follow-Up Adherence and Early Complication Management
Follow-up reviews are designed to identify delayed healing, early pigment changes, or abnormal inflammatory responses. Skipping reviews removes the opportunity to intervene before complications become established. Acne scar resurfacing protocols are staged, and treatment spacing is adjusted based on individual healing response. Laser clinics assess whether erythema has stabilised, whether texture recovery is progressing evenly, and whether pigment modulation is required before proceeding with additional sessions. Patients who self-manage complications without clinical input often worsen outcomes by introducing unsuitable products or delaying necessary medical-grade interventions. Consistent follow-up allows clinicians to adjust parameters, modify aftercare plans, and reduce cumulative risk over multiple resurfacing sessions.
Conclusion
Aftercare determines whether acne scar resurfacing delivers controlled remodelling or prolonged recovery with secondary complications. Sun protection, barrier-safe skincare, activity modification, and follow-up adherence each influence healing stability and surface outcomes. Patients who treat aftercare as optional increase the likelihood of pigment changes, delayed healing, and inconsistent texture correction. Laser clinics structure aftercare protocols to reduce avoidable risks, but outcomes depend on whether patients apply these controls consistently beyond the clinic setting.
Contact Veritas Medical Aesthetics and let us help you plan your recovery while also launching your session.